|
The medicine induces what has been called dependence but might be better called a stress syndrome Stress syndromesĭrug withdrawal arises after the medicine has produced a change in the body aside from its effect on the illness. Motivational interviewing can do something to establish whether someone is willing to face the difficulties of withdrawal. A behavioral activation program or physiotherapy may be appropriate but sitting down to talk through your problems with someone is more likely to make things worse. There is a common assumption that drug withdrawal is a mental phenomenon and can be treated with psychotherapy. In the case of antidepressants, dizziness likely arises from the inner ear and a variety of head zaps and other disturbances come from the blood vessels to the scalp, eyes and other areas of the head. Some of the most distressing effects of drug withdrawal even ones that appear to come from the head in all likelihood do not come from the brain. The effects of stopping drugs may arise from areas other than the brain. It is good marketing that gets us to think that cardiac drugs aren’t also altering our behavior. Similarly most of our cholesterol and lipids are in our brains rather than in our blood. There is a myth that SSRIs act on the brain only when in fact 95% of our serotonin lies outside our brains. It should be assumed that all drugs act on everything. This is almost certainly not the explanation in most cases. Drugs with a short half-life supposedly cause more problems than those with a long half-life. If companies ever offer explanations it is usually in terms of the half-life of the drug. 
Until the pharmaceutical industry and academia concede there can be problems it is difficult to investigate agents and find out which is the worst and why. 
In the case of antipsychotics clozapine, olanzapine and trifluoperazine are much worse than haloperidol or sulpiride.ĭenial is not helpful. In the case of sodium channel blockers lamotrigine appears to be the worst. If a drug group is linked to withdrawal problems, there are likely to be some drugs within the group that are worse than others. We need information on and strategies specific to each drug group. The antidepressants include five groups: serotonin reuptake inhibitors, norepinephrine reuptake inhibitors, receptor blockers, monoamine oxidase inhibitors and others. 
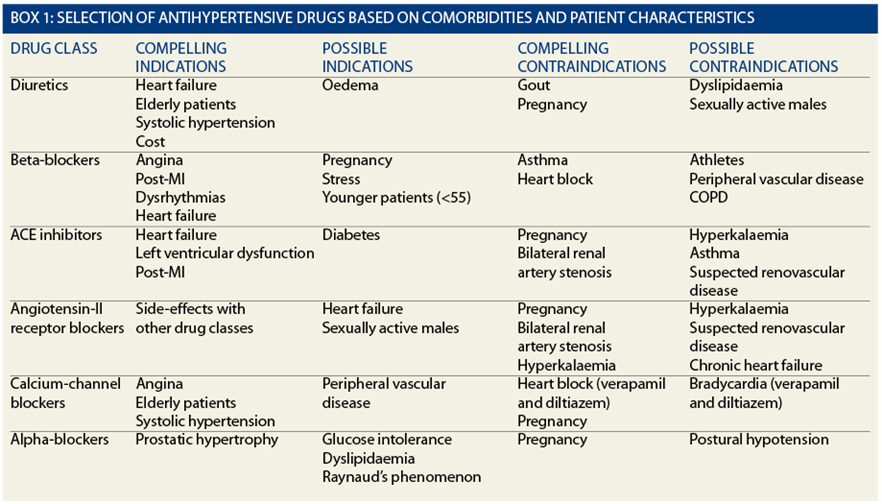
The anticonvulsants in turn break down into 4 groups – sodium channel blockers, drugs that act on the GABA system, carbonic anhydrase inhibitors and at least one more group with an unknown mechanism of action. The mood-stabilizers break-down into at least 3 different drug groups – antipsychotics, anticonvulsants and lithium. This is also important because some drug groups may be used for a few different reasons thiazides are used for hypertension and heart failure and if they cause withdrawal for one use they are likely to cause it for others also. When asking the question about dependence, we need to ask do beta-blockers cause dependence and withdrawal rather than do antihypertensives cause withdrawal. Thus within the antihypertensives, there are thiazides, beta-blockers, ACE-inhibitors and others. Within each apparent treatment group, there may be a number of drug groups. There are a number of principles that can be outlined to cover the management of these various conditions. The commonest queries to RxISK have been about dependence on and withdrawal from a range of drugs, from statins to anticonvulsants.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
